IMPORTANT SAFETY INFORMATION
Contraindications
Otezla is contraindicated in
patients with a known
hypersensitivity to apremilast or to any of the excipients in the formulation
Warnings and Precautions
Hypersensitivity:
Hypersensitivity reactions, including angioedema and anaphylaxis, have been reported during postmarketing
surveillance. If signs or symptoms of serious hypersensitivity reactions occur, discontinue Otezla and
institute appropriate therapy
IMPORTANT SAFETY INFORMATION
Contraindications
- Otezla is contraindicated in patients with a known hypersensitivity to apremilast or to any of the excipients in the formulation
Warnings and Precautions
- Hypersensitivity: Hypersensitivity reactions, including angioedema and anaphylaxis, have been reported during postmarketing surveillance. If signs or symptoms of serious hypersensitivity reactions occur, discontinue Otezla and institute appropriate therapy
- Diarrhea, Nausea, and Vomiting: Cases of severe diarrhea, nausea, and vomiting were associated with the use of Otezla. Most events occurred within the first few weeks of treatment. In some cases, patients were hospitalized. Patients 65 years of age or older and patients taking medications that can lead to volume depletion or hypotension may be at a higher risk of complications from severe diarrhea, nausea, or vomiting. Monitor patients who are more susceptible to complications of diarrhea or vomiting; advise patients to contact their healthcare provider. Consider Otezla dose reduction or suspension if patients develop severe diarrhea, nausea, or vomiting
- Depression: Carefully weigh the risks and benefits of treatment with Otezla for patients with a history of depression and/or suicidal thoughts/behavior, or in patients who develop such symptoms while on Otezla. Patients, caregivers, and families should be advised of the need to be alert for the emergence or worsening of depression, suicidal thoughts or other mood changes, and they should contact their healthcare provider if such changes occur
- Plaque Psoriasis: Treatment with Otezla is associated with an increase in depression. During clinical trials in patients with moderate to severe plaque psoriasis, 1.3% (12/920) of patients
reported depression compared to 0.4% (2/506) on placebo. Depression was reported as serious in 0.1% (1/1308) of patients exposed to Otezla, compared to none in placebo-treated patients (0/506). Suicidal behavior was
observed in 0.1% (1/1308) of patients on Otezla, compared to 0.2% (1/506) on placebo. One patient treated with Otezla attempted suicide; one patient on placebo committed suicide
- Psoriatic Arthritis: Treatment with Otezla is associated with an increase in depression. During clinical trials, 1.0% (10/998) reported depression or depressed mood compared to 0.8%
(4/495) treated with placebo. Suicidal ideation and behavior was observed in 0.2% (3/1441) of patients on Otezla, compared to none in placebo-treated patients. Depression was reported as serious in 0.2% (3/1441) of
patients exposed to Otezla, compared to none in placebo-treated patients (0/495). Two patients who received placebo committed suicide compared to none on Otezla
- Behçet’s Disease: Treatment with Otezla is associated with an increase in depression. During the clinical trial, 1% (1/104) reported depression or depressed mood compared to 1% (1/103)
treated with placebo. No instances of suicidal ideation or behavior were reported in patients treated with Otezla or treated with placebo
- Weight Decrease: Monitor body weight regularly; evaluate unexplained or clinically significant weight loss, and consider
discontinuation of Otezla
- Plaque Psoriasis: Body weight loss of 5-10% occurred in 12% (96/784) of patients with moderate to severe plaque psoriasis treated with Otezla and in 5% (19/382) of patients treated with
placebo. Body weight loss of ≥10% occurred in 2% (16/784) of patients treated with Otezla compared to 1% (3/382) of patients treated with placebo
- Psoriatic Arthritis: Body weight loss of 5-10% was reported in 10% (49/497) of patients taking Otezla and in 3.3% (16/495) of patients taking placebo
- Behçet’s Disease: Body weight loss of >5% was reported in 4.9% (5/103) of patients taking Otezla and in 3.9% (4/102) of
patients taking placebo
- Drug Interactions: Apremilast exposure was decreased when Otezla was co-administered with rifampin, a strong CYP450 enzyme inducer; loss of Otezla efficacy may occur. Concomitant use of Otezla with CYP450 enzyme inducers (e.g., rifampin, phenobarbital, carbamazepine, phenytoin) is not recommended
Adverse Reactions
- Plaque Psoriasis: The most common adverse reactions (≥5%) are diarrhea, nausea, upper respiratory tract infection, and headache, including tension headache. Overall, the safety profile of Otezla
in patients with mild to moderate plaque psoriasis was consistent with the safety profile previously established in adult patients with moderate to severe plaque psoriasis
- Psoriatic Arthritis: The most common adverse reactions (≥5%) are diarrhea, nausea, and headache
- Behçet’s Disease: The most common adverse reactions (≥10%) are diarrhea, nausea, headache, and upper respiratory tract infection
Use in Specific Populations
- Otezla has not been studied in pregnant women. Advise pregnant women of the potential risk of fetal loss
Please click here for the full Prescribing Information.
INDICATIONS
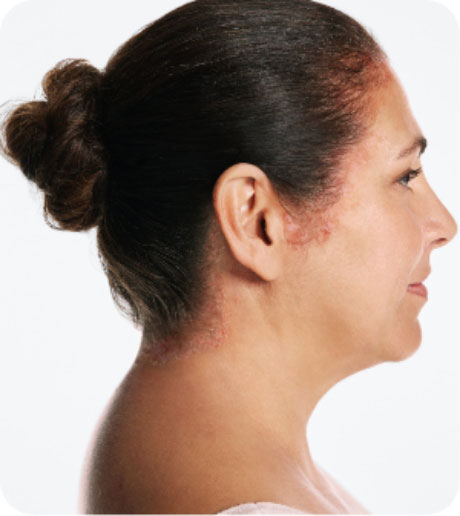
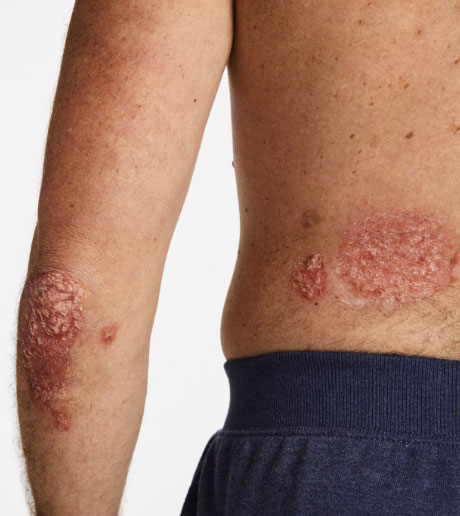
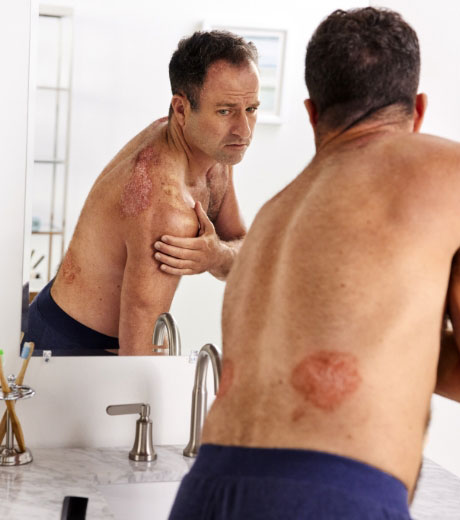
Otezla® (apremilast) is indicated for the treatment of adult patients with plaque psoriasis who are candidates for
phototherapy or systemic therapy.
Otezla is indicated for the treatment of adult patients with active psoriatic arthritis.
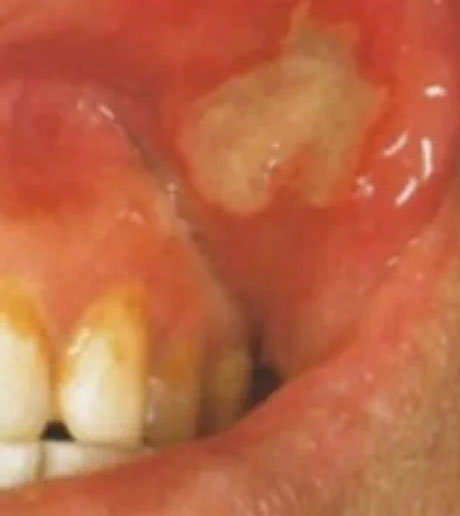
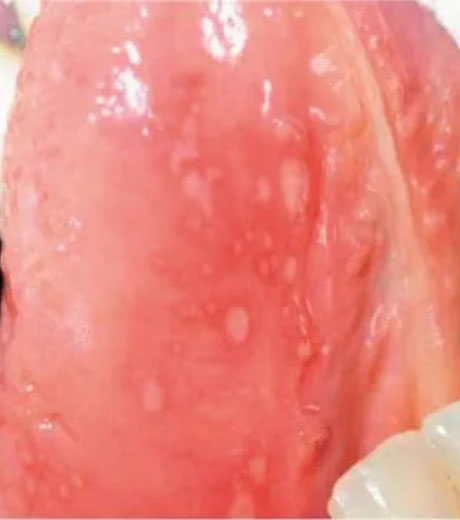
Otezla is indicated for the treatment of adult patients with oral ulcers associated with Behçet’s Disease.